Capsule Endoscopy
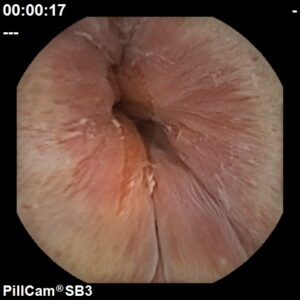
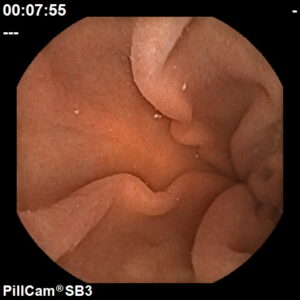
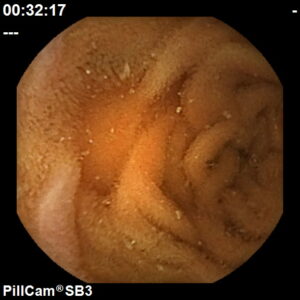
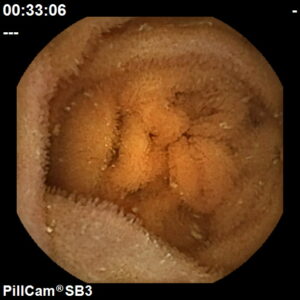
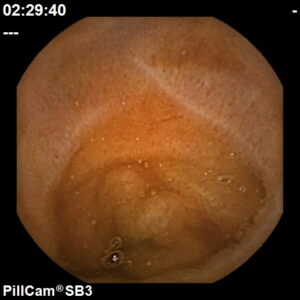
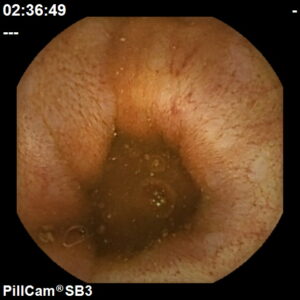
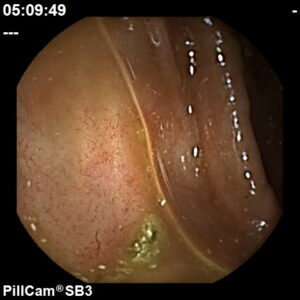
A procedure used to diagnose and monitor diseases of the small intestine with a small, disposable, pill sized camera.
We use the PillCam SB3, a next generation HD capsule that provides exceptional image quality and natural tissue colours for greater diagnostic accuracy.
Because of changes to the MBS that substantially reduced the rebate for this procedure we have been forced to charge a small gap for capsule endoscopy; $150 for our patients, and $300 for externally referred patients.
How to book, in 3 easy steps
1
Complete our booking form
Ready to make an appointment? Simply complete our Book Appointment form and select your appointment type.
2
Expect our phonecall or email
Our Reception team will receive your completed form and discuss with our doctors. We'll contact you to arrange an appointment.
3
Prepare for your appt
Make sure you have a referral from your doctor and bring all recent blood tests and scans. Read our Patient Info page for more information.